“Honestly, the mobile clinic is our only hope of adequate access to healthcare.”
21 April 2021


As a result, whereas Israeli settlers have unimpeded access modern clinics and hospitals, the approximately 298,000 residents of Palestinian communities entirely or partially in Area C have severely restricted access to healthcare.

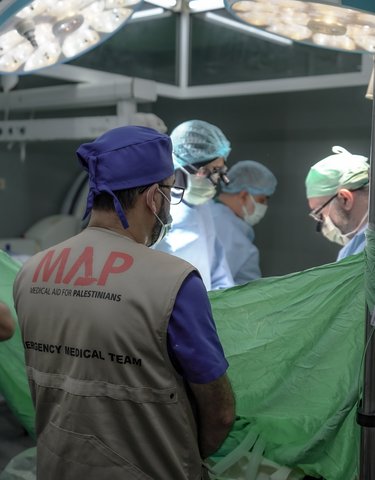
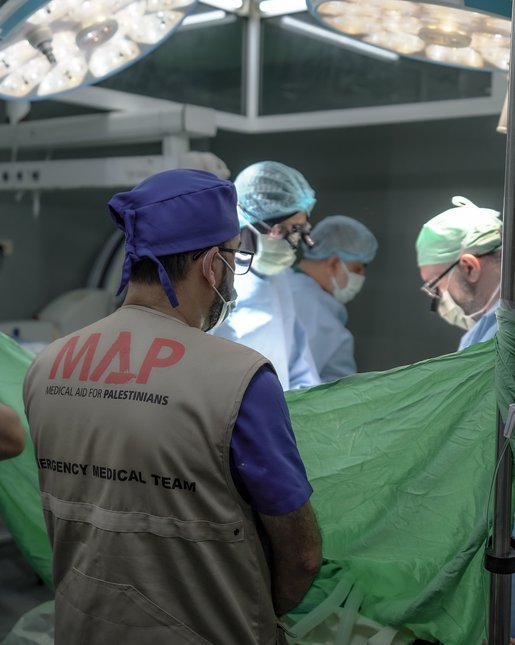
Medical Aid for Palestinians (MAP) partners with the Palestinian Medical Relief Society (PMRS) to provide a mobile clinic for marginalised Palestinian communities facing these challenges in the southern West Bank. On a recent visit to the villages of Deir al ‘Asal and Deir al Reish, both located around 15km southwest of Hebron city, one of the clinic's doctors, Dr Sahar Al Sulibe, described why the mobile clinic’s services are so essential:
“Most of the communities that we visit are marginalised, isolated and located far from the nearest medical centres. The presence of the illegal settlements also restricts the movement of community members, medical staff and even ambulances – in some communities, patients must cross two checkpoints to reach the nearest permanent clinic. So our visits alleviate the costs and challenges of traveling to the city centre for care.”
These communities also contend with poor living conditions, including poverty, persistent threats of demolitions and settler violence, and restricted access to basic needs like clean water and electricity. These conditions have exacerbated the impact of the COVID-19 pandemic on the health and wellbeing of residents: “Poverty and unemployment rates have increased, leading to the increase of gender-based violence, mental distress and malnutrition,” Dr Sahar explained. “We have also encountered an increase of the number of anaemic children.”
The mobile clinic consists of a team of seven: a general practitioner (GP), lab technician, gynecologist, two health workers, a driver and a rehabilitation specialist.

Mobile clinic supervisor Dr Suhail Aqabna described some of the essential services they provide on their weekly visits: “The mobile clinic doesn’t only provide medications and regular follow-ups for patients, but also delivers workshops and trainings on different topics, such as reproductive health, gender, early marriage, first aid, or issues we feel are relevant to each community. We take care to build relations with the community so we can monitor and assess their needs.”
Fo’ad Amro, who lives in the Deir al Reish, described how valuable these services are to his community: “Every week, we wait patiently for the mobile clinic to arrive to our village. Due to our living circumstances – including the restrictions to our movement, the lack of access to medical services, and the high unemployment and poverty rate – we are completely reliant on the mobile clinic.”
“The PMRS staff have built a good relationship with us. They know the medical records of most of the community members here. Honestly, the mobile clinic is our only hope of adequate access to healthcare.”
You can support our mobile clinic by making a donation to MAP today: